Breast density
If your breasts are dense it can also be difficult to see cancer in your mammogram picture. This is because cancer cells and dense breast tissue both show up white on a mammogram - therefore the cancer can be hidden by islands of dense tissue or difficult to see if the breasts are extremely dense.
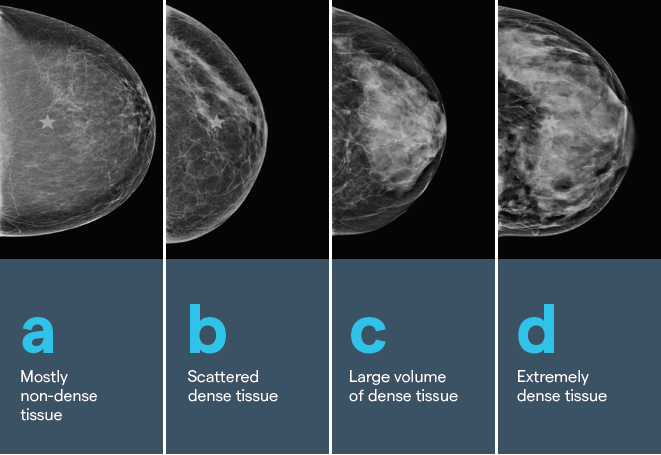
Density has four grades, that are determined by the amount of fibrous and glandular tissue in the breast.
Image A: The breast is composed almost entirely of fat. Fibrous and glandular tissue makes up less than 25 % of the breast. About 1 in 10 women have this.
Image B: 25 to 50 % of the breast is made up of fibrous and glandular tissue. About 4 in 10 women have this.
Image C: 51 to 75 % of the breast is made up of fibrous and glandular tissue. Sometimes described as moderate density. About 4 in 10 women have this.
Image D: The breast tissue is extremely dense, with 75% or more fibrous and glandular tissue. About 1 in 10 women has this.
If your mammogram report describes moderate or extreme density the following applies. Breastscreen Aotearoa (BSA) recommend that if you have an average risk of breast cancer, then 2 yearly mammograms are all that is required for screening. However, if you have a very strong family history of breast cancer or carry a genetic mutation like BRCA, it is recommended that your GP organises an individual plan for you in conjunction with a breast specialist.
Breast tissue is formed by supportive tissue (known as fibroglandular tissue) and fatty tissue. Dense breasts have more of this supportive tissue and non-dense breasts have more fatty tissue. Having dense breasts is actually quite common – research indicates that it affects almost half of all women. Whilst it’s not clear why some women have dense breast tissue and others don’t, it is understood that you are more likely to have dense breast tissue if you are younger, have a lower Body Mass Index (BMI) or take hormone replacement therapy.
Take a look at our webinar on breast density which answers the questions what breast density is and why it is important, how it is measured and how it might affect a diagnosis of breast cancer.
Duct ectasia
Breasts are made up of lobules (milk-producing glands) and ducts (tubes that carry milk to the nipple). These are surrounded by glandular, fibrous and fatty tissue.
As a woman gets nearer to menopause and the breasts age (from 35 years onwards) the ducts behind the nipple shorten and widen. Sometimes a fluid is produced that can collect in the widened ducts. Nipple discharge might be thick or watery, green, black or occasionally bloodstained. A lump may be felt behind the nipple due to thickened, scarred tissue. Occasionally the nipple may start to indraw as the ducts shorten. These symptoms need to be thoroughly investigated by mammogram to exclude cancer.
Duct ectasia is more common in people who smoke, although the exact reason for this is unknown.
Radial scar (complex sclerosing lesion)
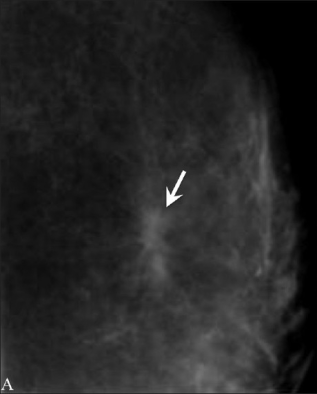
Radial scars are not scarring – they are areas of hardened breast tissue with surrounding abnormal ducts and tissue structures. This mammogram image shows the arrow pointing to a bicycle spoke pattern. Most radial scars will never be felt as a lump. They are usually found on mammogram imaging, however they look similar to cancer, so need to be tested. A core biopsy is taken which involves taking a sample from the center of the radial scar. Removing the scar with surgery is often recommended to make sure the surrounding tissue is normal.
A referral to a breast surgeon is required for further investigation.
Sclerosing adenosis
This is an overgrowth of tissue in the breast lobules. It might not cause any symptoms and in that case, would be found by mammogram. Like the radial scar, it can look like cancer, so needs to be tested.
No treatment is needed but it is associated with a slightly increased risk for developing breast cancer.
Intraductal papilloma (papillary neoplasm)
This is a wart-like growth which develops inside a breast duct close to the nipple. There may be a palpable lump or it might only be detected on a mammogram, and in some cases, it produces a clear or blood-stained nipple discharge. Papillomas are most common in women aged 35-55.
Referral to a breast clinic is needed to rule out breast cancer. Single papillomas with no abnormal cells don’t increase breast cancer risk, but women who have multiple papillomas (papillomatosis) have a slightly higher risk of breast cancer and regular surveillance is advised.
Benign breast calcifications
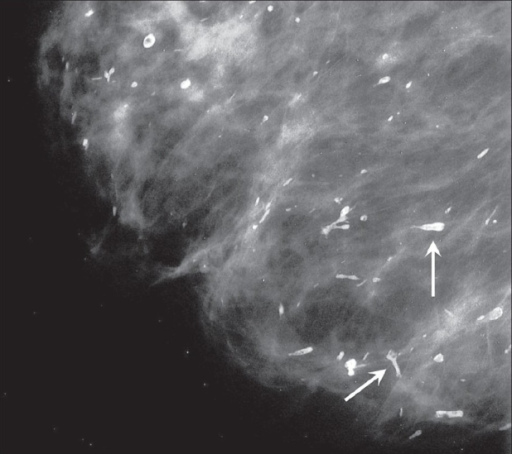
Benign breast calcifications are tiny deposits of calcium in the breast tissue they can be seen as white spots on this mammogram image. They are too small to cause any symptoms so are usually detected as white spots on a mammogram, particularly in women over 50. The majority are not usually visible on an ultrasound scan. They are not related to dietary calcium intake.
Sometimes the presence of breast calcifications can indicate cancer but, in most cases, they are totally harmless. They may be a consequence of natural aging of breast tissue or may result from:
- previous infection
- trauma
- surgery
- cysts,
- fibroadenomas
- radiation therapy.
When calcifications are detected on a mammogram, radiologists examine them closely to assess their size, shape, pattern and distribution. This enables them to distinguish benign calcifications from those which might suggest the presence of cancer or pre-cancer.
Calcifications that are labelled "indeterminate" need further investigation to exclude cancer. This might involve extra magnified mammography views or in some cases a biopsy. Calcifications that are clearly benign don't require any further investigation or treatment.
Fibroadenomas
Fibroadenomas usually present as a lump or a change detected on ultrasound/mammogram. Fibroadenomas can be different in size, with some women having more than one. The only way to know you have a fibroadenoma is to have a sample taken (biopsy).
Fibroadenomas are common and thought to be related to the female hormone estrogen. Hormone levels are higher when we are young, pregnant, breast feeding or taking hormone replacement. Although they can appear at any age, they are more likely when aged 15-40 years.
Fibromas are found in the breast lobule, which is the part of the breast that produces milk. Lobules are made up of glands (that hold the milk), ducts (where the milk travels out of the breast) and fibrous tissue (that holds the breast shape). Fibroadenomas occurs when are tissue in the lobule overgrows and becomes hard.
Most will shrink over time, so are usually left alone. If your fibroadenoma becomes larger or is painful you can speak to a breast specialist about having it removed.
